Most bird bites are not dangerous in the way people fear. For the vast majority of encounters, a bird bite from a pet parrot, a backyard crow, or even a goose causes a sharp sting, maybe a small puncture or bruise, and nothing more serious than a sore spot that heals in a few days. But if a bird bites you, it is still important to clean the wound right away and watch for infection <a data-article-id="8FF908E8-1B67-49A3-B5BF-67C68048F287">sharp sting</a>. That said, bird bites are not completely harmless either. The real risk is not venom or brute force, it is infection. A bird's beak can introduce bacteria into skin that may cause a local infection if the wound is not cleaned promptly and properly. In rare cases, those infections escalate. So the honest answer is: bird bites are usually minor, but they deserve basic first aid and a clear-eyed look at when something more is needed. If you are also wondering what a bird bite is called, many people use the term “bird bite” or “animal bite” in general, but the medical concern is the same: possible infection.
Is Bird Bite Dangerous? First Aid, Risks, and When to Get Help
How dangerous are bird bites, really?
It depends on the bird, the depth of the wound, and how quickly you deal with it. A small finch nibbling a finger is not in the same category as a large macaw clamping down on a knuckle or a wild bird delivering a deep puncture. Research on animal bite wound microbiology confirms that human infections from bird bites are generally minor and rare, but documented cases of serious infection do exist. The CDC's Yellow Book explicitly notes that bite and scratch wounds can result in serious illness or death in humans through zoonotic infection, and StatPearls categorizes animal bites as posing complex clinical risk including tissue damage and disease exposure. Those are worst-case scenarios, but they are not myths either, which is why treating even a modest bird bite with some respect makes sense.
The location and severity of the bite changes the equation significantly. A superficial nick on the forearm is a different story from a deep puncture wound on your hand or a bite near your face. Bites on the hand carry higher infection risk partly because the anatomy there is tight, tendons, joints, and tendon sheaths sit close together with limited blood supply, making it easier for bacteria to spread before you notice a problem. The CDC's guidance on wound management puts animal bites in the category of 'dirty or major wounds' because of saliva and contamination risk, which is a useful baseline for thinking about how seriously to take any bite regardless of which species was responsible.
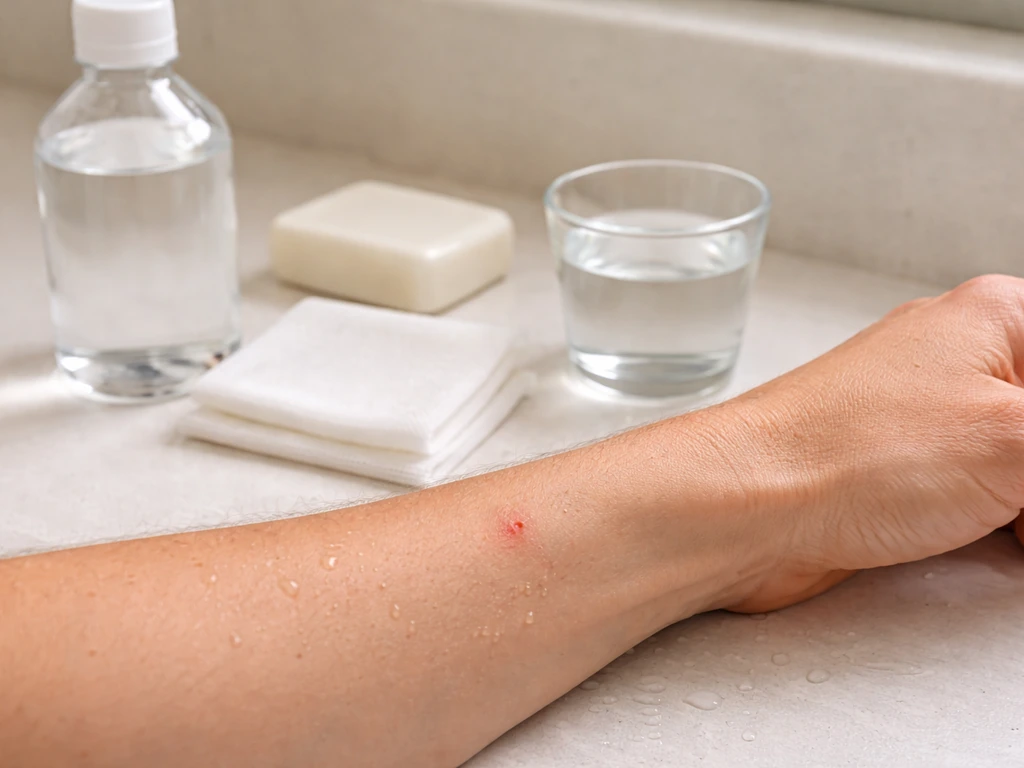
What to do right after a bird bites you

Act immediately, even if the wound looks minor. The goal in the first few minutes is to reduce bacterial load in the wound before it has a chance to establish itself in tissue.
- Wash the wound thoroughly with soap and water for at least a few minutes. This is the single most important step — running water and soap physically removes bacteria from the wound site. Do not skip this even if the bite looks small.
- Control any bleeding with gentle, direct pressure using a clean cloth or gauze. Most bird bites stop bleeding on their own fairly quickly.
- Apply an antibiotic ointment (like bacitracin or a triple antibiotic product) to the cleaned wound if you have one available.
- Cover the wound with a clean bandage or dressing to protect it from further contamination.
- Watch it closely over the next 24 to 48 hours for any signs of infection, even if it felt minor at the time.
Both the Mayo Clinic and the American Red Cross first-aid guidelines line up on these core steps: wash, cover, monitor. The washing step is non-negotiable. A bird's beak is not sterile, and the mouth and beak environment can carry bacteria that do not belong in a wound.
Signs that mean you need medical care now
Some bird bites need a doctor, not just a bandage. Go to urgent care or an emergency room if you notice any of the following:
- Redness spreading outward from the wound, especially if it is growing visibly over a few hours
- Red streaks radiating away from the bite (this is a classic warning sign of lymphangitis, which means infection is traveling through the lymphatic system — the Cleveland Clinic classifies this as a call-your-provider-immediately situation)
- Pus or discharge from the wound
- Increasing warmth and swelling around the bite
- Fever or flu-like symptoms developing after a bite
- Severe or worsening pain out of proportion to the wound size
- Difficulty moving fingers or other digits near the bite site
- Any bite on the hand, face, or near a joint
- Deep puncture wounds, especially those that may have reached bone or joint
- The wound was caused by a wild or stray bird with unknown health status
StatPearls notes that infection signs after animal bites can appear quickly. With Pasteurella bacteria in particular, symptoms like significant local inflammation and swelling can show up within 8 to 12 hours and often within 24 hours. If you are watching a wound and it starts looking worse rather than better within that window, that is your cue to stop waiting and get it evaluated.
What germs are actually involved and how likely is infection?

The most commonly discussed bacteria in bird and animal bite wound infections are Pasteurella species and Staphylococcus aureus, both flagged by the CDC as pathogens associated with zoonotic bite and scratch exposures. Pasteurella in particular tends to cause aggressive skin and soft tissue infections, with local lymphadenopathy (swollen lymph nodes), pain, and swelling developing fast. Staph infections are generally more familiar territory for most people, they can cause localized skin infections that, if untreated, can spread.
There is also Chlamydia psittaci, the bacterium responsible for psittacosis. This is primarily a respiratory illness associated with inhaling particles from bird droppings or feathers, but the CDC notes that birds can infect people through bites and beak-to-mouth contact, even if that is less common than the airborne route. People who handle pet birds, especially parrots and cockatiels, or who work with poultry, are considered higher risk. The illness ranges from mild to severe and can look like a bad flu or pneumonia.
In terms of overall infection probability, the numbers from the animal bite literature put things in perspective. Research on dog bites (the most studied animal bite category) shows that getting antibiotic treatment within 6 hours of a bite cuts infection risk to around 8 percent, while delaying treatment pushes that risk toward 59 percent. That is a huge difference and a strong argument for not brushing off a bite and hoping for the best. Time to care is one of the most controllable factors you have.
Rabies and tetanus after a bird bite
Rabies: not a risk from birds
Here is where some common internet worry can be put to rest directly. Birds cannot get rabies and cannot transmit rabies to humans. Rabies is a viral disease of mammals, transmitted through the bite of an infected mammal. The DC Department of Health explicitly lists birds among the animals that cannot get or spread rabies. The CDC defines rabies risk in terms of mammalian reservoirs like bats, raccoons, foxes, and skunks. If a bird bites you, rabies post-exposure prophylaxis (PEP) is not indicated and not something you need to discuss with a clinician in that context.
Tetanus: worth thinking about
Tetanus is a different matter. The CDC categorizes animal bites as 'dirty or major wounds' because saliva is introduced into the wound, and that puts them in the higher-risk wound category for tetanus prophylaxis planning. If your bird bite leaves a wound, tetanus prophylaxis may be recommended based on your vaccination history. Whether you need a booster or tetanus immune globulin (TIG) depends on your vaccination history. The general framework from the CDC and the Minnesota Department of Health is this: if you have had a complete primary series and your last booster was within the past 5 years, you are typically covered for even a dirty wound. If you have had fewer than 3 documented doses, or your vaccination history is unknown, TIG plus a tetanus toxoid vaccine is recommended for higher-risk wounds. If it has been more than 5 years since your last booster, a booster shot is worth discussing with a clinician after any significant animal bite. When you go to urgent care after a bird bite, this is a routine question they will ask about, just be ready with your vaccination history if you know it.
What makes one bird bite more dangerous than another?
Not all bird bites are created equal, and a few factors reliably shift the risk level up or down.
| Factor | Lower Risk | Higher Risk |
|---|---|---|
| Bird size and beak strength | Small birds (finches, budgies, canaries) | Large birds (macaws, cockatoos, geese, raptors, cassowaries) |
| Wound depth | Superficial scratch or surface abrasion | Deep puncture, laceration, or wound near bone/joint |
| Location on body | Trunk, arms, legs (away from joints) | Hand, fingers, face, scalp, near joints |
| Bird health status | Healthy, vaccinated, observable pet bird | Wild bird, bird showing signs of illness, unknown health history |
| Time to first aid | Cleaned within minutes of the bite | Delayed cleaning or no immediate wound care |
| Your health status | Otherwise healthy adult | Immunocompromised, diabetic, elderly, or on medications that affect immunity |
StatPearls specifically identifies hand location and bite size exceeding 3 cm as factors that increase infection risk from animal bites. Your own immune status matters too. People who are immunocompromised, diabetic, or on certain medications are at higher risk of a minor wound turning into a significant infection. If that describes you, the threshold for seeking medical care after a bird bite should be lower, meaning you get it checked out even when it looks mild.
How to prevent bird bites in the first place

Pet bird owners
Most pet bird bites happen during handling, often when a bird is startled, stressed, overstimulated, or simply communicating that it wants to be left alone. Learning your bird's body language, pinned eyes, raised feathers, lunging posture, goes a long way. The CDC's Healthy Pets guidance for bird owners reinforces good hygiene after handling birds and their equipment, and notes that beaks can cause real damage. Specific steps that help:
- Never reach into an enclosure with a stressed or agitated bird without reading its body language first
- Avoid putting your face near large parrots, especially unfamiliar ones — facial bites can be serious
- Teach 'step up' commands from a young age to reduce the need for forced handling
- Wash hands thoroughly after handling birds, their food and water dishes, and cage accessories
- If a bird is nesting or brooding, give extra space — hormonal birds bite more aggressively and unpredictably
Wild birds and outdoor encounters
Wild birds bite humans most often when cornered, protecting a nest, or being handled during rescues or veterinary care. Geese, swans, and corvids can bite with surprising force. If you are approaching an injured wild bird, use thick gloves or a towel to create a barrier. Never try to handle a raptor (hawk, owl, eagle) without proper training and protective equipment, their talons are the real threat, but the beak can do damage too. Give nesting birds a wide berth during breeding season, especially colonial nesters or birds known to dive-bomb (red-winged blackbirds are the classic example in North America).
Aviation and professional settings
For aviation professionals and people who work in environments where birds are present occupationally, the focus is typically on bird-strike hazard mitigation at the systems level rather than individual bite risk. That said, wildlife control personnel, biologists banding birds, and airport wildlife managers who handle birds directly should treat any bite as a potential infection exposure. Use appropriate PPE when handling birds in professional contexts, follow your organization's bite-reporting and wound-care protocols, and do not let a 'small' bite go undocumented or untreated in a workplace setting. The CDC's principle applies here: a bird appearing healthy is not a guarantee it is free of transmissible pathogens.
The bottom line on bird bite risk
Bird bites sit in the 'usually minor, occasionally serious' category. If you are wondering whether do bird bites hurt, the most common result is a sharp sting that may leave a small sore spot for a few days <a data-article-id="4B8DCC1C-C3E8-4F91-A86B-2A5AEFCB712C">usually minor, occasionally serious</a>. The bite itself is rarely structurally devastating unless you are dealing with a large bird. The real danger is what can get into the wound, how fast, and whether you address it promptly. Wash the wound immediately, watch for infection signs over the next 24 to 48 hours, and know when to get medical help. If you are also wondering what happens if a bird gets your hair, the main concern is still the same as with any bird contact, possible skin irritation and infection risk from tiny bites or scratches. If you are also wondering what happens if a bird scratches you, the main concern is still the same as with any bird contact, possible skin irritation and infection risk from tiny bites or scratches. You do not need to worry about rabies after a bird bite, but tetanus prophylaxis is worth confirming if your vaccination history is out of date. People who are immunocompromised or who receive a bite on the hand or face should seek evaluation even without obvious red flags. Everything else being equal, quick and thorough first aid is your best protection.
FAQ
If it barely broke the skin, is a bird bite still dangerous?
Yes, the risk is usually low but not zero. Even tiny punctures or scratches can introduce bacteria, and infections from bite wounds can start within about 24 hours. If you cannot fully wash the area right away, clean it as soon as possible and monitor closely, especially for redness spreading, increasing pain, or swelling.
Should I apply antibiotic ointment or leave the wound alone after a bird bite?
A thin layer of topical antibiotic can be helpful for minor superficial wounds, but washing is the key step. Avoid soaking the wound in baths, hydrogen peroxide, or harsh disinfectants repeatedly, since they can irritate tissue. Covering with a clean dressing and changing it daily helps keep the area protected while you watch for infection.
How do I tell normal bruising from an infection after a bird bite?
Bruising and mild soreness usually improve day by day. Infection is more likely when redness enlarges, warmth increases, swelling worsens, pain becomes more intense after an initial period, pus appears, or lymph nodes in the arm or neck area become tender or swollen. Also take early worsening within 8 to 24 hours seriously.
Do I need stitches or medical closure after a bird bite?
Sometimes, but not automatically. Deep puncture bites on the hand often should not be tightly closed because trapped bacteria can worsen infection risk. Clinicians decide based on depth, time since injury, location, and whether it can be thoroughly irrigated.
Is it okay to drain the wound or squeeze out blood after a bird bite?
No. Squeezing or digging at the puncture can push bacteria deeper and cause more tissue damage. Instead, wash under running water, remove visible debris gently, and use pressure only if bleeding does not stop after several minutes.
What if the bird bite happened at work or from a wild bird, do I treat it differently?
Treatment steps are similar, but documentation and follow-up matter more. Report the incident per workplace protocol, ensure you receive wound care evaluation if it was a deep bite or hand or face injury, and consider occupational risk if you handle wildlife or animals regularly.
Can I get tetanus from a bird bite if I am fully vaccinated?
If you completed the primary series and had a booster within the last 5 years, you are often covered even for higher-risk wounds. If your vaccine history is unknown, incomplete, or the last booster was more than 5 years ago, a clinician may recommend a booster and possibly tetanus immune globulin for protection.
Is rabies a concern after a bird bite?
In general, rabies post-exposure prophylaxis is not indicated after a bird bite because birds are not considered rabies-transmitting mammals. The more practical medical priorities are wound infection prevention, tetanus status, and evaluation based on where and how deeply the bird injured you.
How soon should I seek urgent care after a bird bite?
Go sooner if the bite is on the hand or face, involves a deep puncture, or you are immunocompromised or diabetic. Even without those factors, if symptoms are not improving or are getting worse within about 24 hours, get evaluated promptly rather than waiting several more days.
If my bird bites me repeatedly, can I reduce risk without changing my bird?
Often yes. Review triggers like overstimulation, pinned eyes, raised feathers, lunging, or startling. Use calmer handling routines, avoid putting hands near the beak during stress moments, and sanitize equipment afterward. If bites happen during routine care, ask an avian vet or qualified trainer for tailored behavior and handling strategies.

