Most bird bites are minor: a small puncture, some bleeding, and a bruised ego. If you get scratched, you should still clean the area right away and watch for signs of infection, just like you would after a minor bite bird scratches. If you are wondering what a bird bite is called medically, it is typically treated as an avian bite wound. If you are wondering whether a bird bite actually hurts, the answer is that pain can range from mild soreness to sharp, throbbing discomfort depending on the depth and location of the bite do bird bites hurt. But even a bite that looks trivial can introduce bacteria deep into tissue, and a few situations (deep punctures, wild bird bites, bites on the hands or face) genuinely need prompt medical attention. The right move is to clean the wound immediately, watch it closely for 48 to 72 hours, and know the handful of signs that mean you should see a clinician the same day. That is why bird bite risk depends on where and how deep it was, and why some bites can be dangerous even if they seem minor at first is bird bite dangerous.
What Happens If a Bird Bites You: What to Do Next

What bird bite injuries actually look like

Bird bites tend to fall into a few categories depending on the species and how the bite happened. StatPearls classifies bite wounds as some combination of laceration, crush injury, avulsion, and puncture, and bird bites hit all four types depending on beak shape and force. A small finch or parakeet usually leaves a shallow puncture or a pinch mark. A parrot, macaw, or cockatoo can deliver real crush force and create a deep puncture or a torn flap of skin. Wild birds like geese, swans, or raptors can produce genuine lacerations and bruising. The deceptive part is that a clean-edged puncture from a pointed beak can track bacteria surprisingly deep while looking minor on the surface. The CDC specifically flags this: a bird's beak can cause serious injury even when the bite doesn't look deep.
Location matters a lot for how seriously you treat the bite. StatPearls lists the hands, feet, face, and any puncture wound as high-risk areas. Your hands are the most common target and also the worst place to get an infected bite: tendon sheaths, joints, and small spaces between bones can trap bacteria with very little room for your immune system to respond. A bite on a finger that gets infected can escalate to cellulitis, abscess, or lymphangitis (infection tracking up the lymph channels) faster than bites elsewhere on the body.
Immediate first aid: what to do right now
The single most important thing you can do in the first few minutes is wash the wound thoroughly. Johns Hopkins recommends running water over the wound under faucet pressure for at least 5 minutes with soap, and explicitly advises not scrubbing hard, since scrubbing can bruise tissue and push bacteria deeper. MedlinePlus suggests 3 to 5 minutes for minor bites; LA County Public Health extends that to 15 minutes. The conservative choice is to go longer rather than shorter. Use mild soap and the warmest running water you can tolerate.
- Control any bleeding first by applying firm, direct pressure with a clean cloth. For most bird bites, bleeding stops within a few minutes.
- Wash the wound under running water with soap for at least 5 minutes. Do not scrub aggressively.
- After washing, apply a thin layer of antibiotic ointment and cover with a clean bandage (Mayo Clinic and CDC both recommend this step for minor wounds).
- Write down the time, the bird species if you know it, and whether the bird was wild, a stranger's pet, or your own.
- Decide whether you need same-day medical evaluation using the criteria below.
If the wound is on your hand, involves a deep puncture, won't stop bleeding after 10 to 15 minutes of pressure, or was from a wild bird, go ahead and get it evaluated today. Do not wait for infection signs to appear before calling a clinician.
Wild bird vs. pet bird bites: the risk differences are real

The source of the bite changes how you think about follow-up. A bite from your own healthy, vet-checked pet bird carries the lowest risk profile: you know the bird's history, it's unlikely to be carrying anything exotic, and psittacosis (caused by Chlamydia psittaci) is a possible but uncommon concern that typically spreads through aerosols and droppings rather than bites. The CDC notes that bite and beak-to-mouth contact are less common transmission routes for psittacosis than inhaling contaminated dust, but it's still worth mentioning to a doctor that the bite was from a pet bird.
Wild bird bites are a different calculation. You don't know that bird's health status, and certain situations add considerations beyond simple wound infection. A bite from a wild bird in an area with active avian influenza outbreaks means you should monitor yourself for flu-like symptoms for 10 days after the exposure, per CDC guidance for people with direct contact with sick or dead birds. If the bite involved a bird that seemed sick or was acting abnormally, document that and report it to your local animal control or public health department. In some areas they want to know about bites from wildlife even when the animal appeared healthy.
One thing you do not need to worry about with any bird bite: rabies. Birds cannot get rabies. DC Health and CDC are both clear that rabies is transmitted through the saliva of infected mammals, and birds are not a rabies vector. This is one of the more common pieces of misinformation that circulates after wildlife encounters, and it simply isn't a concern here.
| Factor | Your pet bird | Wild bird |
|---|---|---|
| Bacterial infection risk | Present, but lower if bird is healthy | Present, potentially higher from unknown flora |
| Psittacosis concern | Possible (lower risk via bite) | Lower, but present with some species |
| Avian influenza exposure | Very low for typical pet birds | Report and monitor if bird seemed ill |
| Rabies risk | None (birds cannot get rabies) | None (birds cannot get rabies) |
| Public health reporting | Usually not required | Often required; contact local animal control |
| Vet evaluation of source bird | Recommended if bird seems unwell | Not usually possible |
When to get urgent medical care (and what to tell the clinician)
Go to urgent care or an emergency department the same day if any of these apply: the bite is on your hand, wrist, or face; it's a deep puncture wound that's difficult to clean; you can't stop the bleeding; you're immunocompromised, diabetic, or on medications that affect your immune response; or the bite was from a wild bird that appeared sick. You don't need to wait for infection to develop before seeking care. Hand bites in particular should be evaluated by a clinician because the anatomy makes early infections difficult to detect and fast to escalate.
When you see the clinician, give them these specifics: the type of bird (species if known, wild vs. They will also use your tetanus vaccination history to decide if you need a tetanus shot after a bird bite. pet), when and where the bite happened, what the wound looked like initially, whether you cleaned it and how, your tetanus vaccination history, and any relevant health conditions. This helps them make the right calls on wound management, antibiotics, and vaccine updates. If you are wondering what happens if a bird gets your hair, the same basics apply: clean the area right away and watch for signs of infection, especially if it was a puncture or scratch wound management. If the bird was wild and seemed ill, say that clearly.
Watching the wound over the next 48 to 72 hours
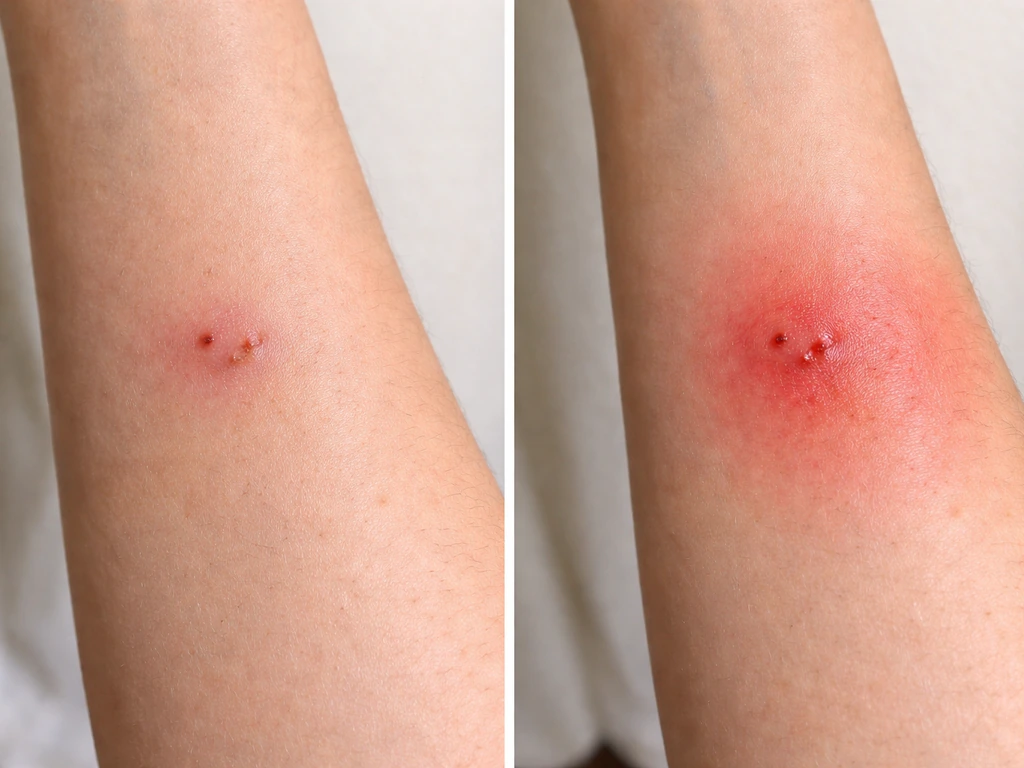
Most infections from bird bites start showing signs within 24 hours, according to the American Academy of Pediatrics, so the first full day after the bite is when you need to be most attentive. Check the wound at least twice a day. The Red Cross and NHS both describe the same warning signs: increasing redness spreading beyond the wound edges, warmth, swelling, pus or cloudy discharge, and red streaks radiating from the wound (a sign of lymphangitis). Fever is a systemic sign that infection has moved beyond the local tissue.
- Increasing redness, especially if it's spreading outward from the bite
- Warmth or swelling that gets worse instead of better
- Pus or any cloudy, smelly discharge
- Red streaks extending from the wound toward the body
- Fever, chills, or flu-like symptoms
- Increasing pain after the first 12 hours (pain should be going down, not up)
Any of those signs means you go back to a clinician the same day, full stop. Cellulitis from a bite wound can escalate to a serious soft tissue infection quickly, especially on the hand. Keep the wound clean, change the bandage daily, and avoid submerging it in water (like a bath or pool) until it's clearly closed and healed.
Tetanus, exposure documentation, and what the clinician will check
Tetanus is a real but preventable concern with bird bites. The CDC classifies penetrating and puncture wounds that involve dirt, feces, or saliva (which includes any animal bite) as high-risk wounds for tetanus. Whether you need a booster or tetanus immune globulin (TIG) depends on two things: the wound type and your vaccination history. If you've had a complete primary series and your last booster was less than 5 years ago, you're generally covered for most wounds. If your last tetanus shot was more than 10 years ago, you'll need a booster regardless of wound type. For high-risk wounds (deep punctures, wounds contaminated with feces or saliva), the threshold is 5 years since the last dose. If you genuinely don't know when you last had a tetanus shot, tell the clinician that directly so they can make the right call. The CDC provides a clear decision framework based on wound type and vaccination history, which your clinician will use.
On rabies: as already noted, birds cannot transmit rabies. You do not need rabies post-exposure prophylaxis (PEP) after a bird bite under any circumstances. Rabies PEP (which involves HRIG and a 4-dose vaccine series per CDC guidance) is reserved for exposures from mammals. If a clinician suggests it for a bird bite, that's worth clarifying.
What you should document: write down the date and time of the bite, the species and whether it was wild or captive, where on your body you were bitten, how the wound initially looked, what first aid you performed, and the behavior of the bird (especially if it seemed sick or was acting abnormally). If a wild bird bit you and you can identify the location, note that too, as some jurisdictions require reporting of wild bird bites. This record helps both your immediate care and any follow-up if symptoms develop later.
How to prevent future bites from your bird or wild birds
Most pet bird bites are preventable with some attention to context and bird behavior. Birds bite for predictable reasons: fear, overstimulation, protecting a cage or a mate, or being handled when they don't want to be. Learning to read your bird's body language (feather position, eye pinning, posture, vocalizations) is the most reliable prevention tool. Never reach into a bird's cage when it's showing signs of agitation, and avoid handling a bird that's molting or unwell, since both states make birds more reactive.
The CDC recommends routine veterinary care for pet birds as part of reducing disease transmission, including through bites and scratches. A well-checked bird is not just healthier but also easier to handle safely. If your bird bites regularly, a certified avian veterinarian or a parrot behavior consultant can identify what's triggering the biting and give you specific strategies.
Around wild birds, the straightforward rule is: don't try to handle them. Birds that allow close human approach are often ill, injured, or habituated in ways that make them unpredictable. If you need to handle a wild bird (to rescue it, for example), use thick gloves and minimal restraint time. Contact a licensed wildlife rehabilitator for anything beyond getting a bird out of immediate danger. For large waterfowl like geese and swans that can genuinely hurt you with their beaks and wings, give them space, especially around nesting season.
FAQ
Should I stop and look for “deep” damage before I treat a bird bite seriously?
Don’t wait for depth to decide. A puncture that looks small can still carry bacteria deep into tissue, especially on the finger, hand, or near joints. Your decision should be based on location and mechanism (puncture vs crush vs laceration), ability to clean it, and whether bleeding was difficult to stop, not just the surface size.
If the bite is just a scratch or pinch, do I still need to watch it for infection?
Yes. Even minor scratches can become infected, so clean it right away and recheck at least twice in the first day and again through 48 to 72 hours. Pay attention to expanding redness, warmth, swelling, pus, red streaks, and fever, since infection can start quickly after bird bites.
Can I use alcohol, hydrogen peroxide, or iodine instead of washing with soap and water?
It’s better to prioritize thorough running water plus mild soap. Harsh antiseptics or aggressive scrubbing can irritate tissue and may not clean as effectively as water pressure. If you want to add an antiseptic, do it after the wound has been washed, not as a substitute.
How long should I keep applying pressure if the bird won’t stop bleeding?
Apply direct pressure for 10 to 15 minutes. If bleeding doesn’t stop after that, get same-day medical evaluation. Persistent bleeding can signal a deeper vessel injury where complications are more likely.
What should I do if the bird bite is on my finger or hand and I can move the finger normally?
Normal movement doesn’t rule out tendon sheath or joint-space involvement. Hand bites are high-risk because infections can spread quickly in tight compartments. If it was a puncture, deep bite, difficult to clean, or getting worse, seek evaluation the same day.
Do I need antibiotics for every bird bite?
Not automatically. Many minor bites are managed with cleaning and monitoring, but clinicians may recommend antibiotics when risk is higher, such as deep punctures, wounds on hands or face, inability to clean well, or bites involving a wild bird. If you’re unsure, the key decision point is whether the bite is high-risk by location and depth.
What tetanus shot should I expect if I have no idea when my last vaccination was?
Tell the clinician you don’t know your last tetanus date. They will use that information plus the wound type to decide whether you need a booster and, for certain high-risk wounds, whether tetanus immune globulin is also needed. Don’t wait for symptoms or try to guess your coverage.
Is rabies a concern after a bird bite?
No. Birds are not a rabies vector, and rabies post-exposure prophylaxis is reserved for exposures from mammals. If a provider suggests rabies treatment for a bird bite, ask them to clarify because it isn’t indicated for bird saliva exposures.
If the bird was a pet, do I still need to see a clinician?
Sometimes, but the threshold is higher for some situations even with a pet bird. Get evaluated the same day if it’s on your hand, is a deep puncture, you cannot clean it easily, bleeding was hard to stop, or you are immunocompromised or diabetic. Also mention whether the bird is healthy and vet-checked to help guide additional considerations.
What extra monitoring is needed after a bite from a wild bird?
Treat it more cautiously. In addition to infection monitoring, document the bird’s appearance and behavior. If the bird seemed sick or acting abnormally, you may need extra public health follow-up and monitoring for flu-like symptoms for about 10 days after direct contact, depending on local guidance.
Should I report a wild bird bite to anyone?
Often, yes. If you can identify the location of the incident or the bird was wild and possibly ill, contact your local animal control or public health department. Some areas request reporting of wild bird bites even when the animal looked healthy.
What if a bird bite got into my clothing or there was feces or saliva involved?
Consider it higher risk for both cleaning needs and tetanus evaluation. Before you cover it, remove contaminated clothing if applicable, wash the wound thoroughly, and make sure you tell the clinician whether feces or saliva contacted the wound. That detail can change tetanus decisions and antibiotic risk assessment.
Is it okay to soak the wound in a bath or pool while it heals?
Avoid submerging it until it is clearly closed and healed. Keep it clean, change dressings daily, and watch for increasing redness, swelling, warmth, pus, red streaks, or fever.
What details should I write down so the clinician can triage me faster?
Record date and time, the bird species (and whether it was wild or captive), exact bite location, what it looked like immediately, what first aid you did (including how long you irrigated and whether you scrubbed), tetanus vaccination history or lack of it, your relevant health conditions, and how the bird behaved (especially any signs it was sick).

